IVF vs. Mitochondrial Replacement: Essential Differences
- Feb 22
- 11 min read

Confronting infertility after 40 can leave even the most determined women searching for hope. When diminished ovarian reserve and questions about egg quality add to your worries, knowing your advanced options becomes vital. Understanding the difference between standard IVF and the specialized approach of mitochondrial replacement therapy gives you the clarity to choose a pathway that addresses not just age but the unique cellular challenges within your eggs, opening doors to possibilities that traditional fertility treatments alone cannot always offer.
Table of Contents
Key Takeaways
Point | Details |
Distinction Between IVF and MRT | Standard IVF uses a woman’s own eggs, while Mitochondrial Replacement Therapy (MRT) replaces faulty mitochondria with healthy ones from a donor for improved embryo viability. |
Reproductive Options for Women Over 40 | Women over 40 may benefit from MRT if mitochondrial dysfunction impairs egg quality, as standard IVF may not resolve fertility issues tied to mitochondrial damage. |
Genetic Counseling Importance | It is essential to request genetic counseling and mitochondrial testing to determine the most suitable fertility treatment based on individual genetic risks. |
Legal and Accessibility Considerations | MRT is restricted in the U.S., requiring international travel for access, thus making cost and logistics significant factors in treatment decisions. |
Defining IVF and Mitochondrial Replacement
Understanding the difference between standard IVF and mitochondrial replacement therapy is crucial for women over 40 evaluating fertility options. Both procedures address infertility, but they work in fundamentally different ways.
In vitro fertilization (IVF) is the foundational fertility treatment. The process involves removing eggs from your ovaries, mixing them with sperm in a laboratory dish, and allowing fertilization to occur outside your body. Once embryos develop to the appropriate stage, your doctor transfers one or more into your uterus for implantation.
IVF addresses infertility caused by various factors:
Low sperm count or poor sperm quality
Blocked fallopian tubes
Ovulation disorders
Unexplained infertility
Advanced maternal age with diminished ovarian reserve
Mitochondrial replacement therapy (MRT) is a specialized form of IVF31487-0) designed for a specific problem: faulty mitochondria within your eggs. Mitochondria are the powerhouses of your cells, providing energy for fertilization, embryo development, and early pregnancy.
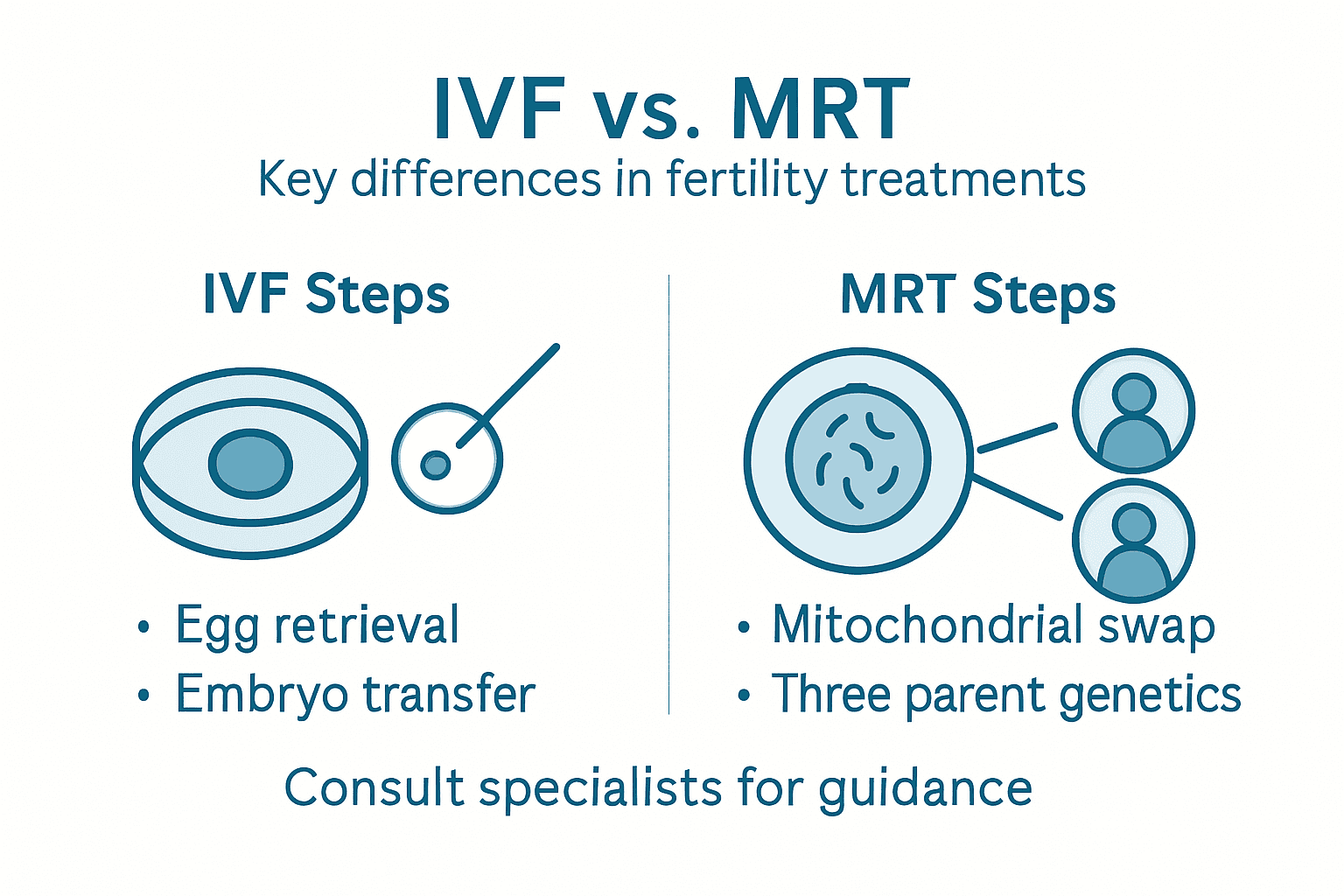
Here’s how MRT differs fundamentally:
Standard IVF focuses on improving fertilization and embryo development with your own genetic material intact.
Mitochondrial replacement therapy removes abnormal mitochondrial DNA from your egg and replaces it with healthy mitochondrial DNA from a donor egg. This creates an embryo with nuclear DNA from both you and your partner, but mitochondrial DNA from a third party.
When mitochondrial dysfunction is the primary fertility barrier, standard IVF alone cannot solve the problem—your eggs lack the cellular energy needed for successful development.
Why does this distinction matter for women over 40? Your eggs naturally accumulate mitochondrial damage over time. Some women experience not just diminished egg quantity, but compromised mitochondrial function that reduces egg quality and implantation success. Standard IVF cannot repair this mitochondrial damage.
Mitochondrial replacement therapy addresses this specific issue by replacing defective mitochondria through specialized egg manipulation. The technique gives your embryos fresh, functional mitochondria from a healthy donor.
Both approaches involve the same basic IVF steps: hormone stimulation, egg retrieval, fertilization, and embryo transfer. The critical difference lies in what happens to your egg before fertilization occurs. In standard IVF, your egg is used as-is. In MRT, it undergoes mitochondrial DNA replacement.
For women with normal mitochondrial function, standard IVF addresses age-related infertility through improved embryo selection and transfer techniques. For women with confirmed mitochondrial dysfunction affecting egg quality, MRT offers a path forward that standard IVF cannot provide.
Pro tip: Request mitochondrial testing as part of your initial fertility evaluation. Understanding whether mitochondrial dysfunction is contributing to your infertility will determine whether MRT or standard IVF represents the appropriate treatment pathway for your specific situation.
Here’s a side-by-side comparison of standard IVF and mitochondrial replacement therapy (MRT) to help clarify their core differences:
Aspect | Standard IVF | Mitochondrial Replacement Therapy (MRT) |
Genetic Contributors | Two (mother & father) | Three (mother, father, donor) |
Targeted Infertility Issues | Broad infertility causes | Mitochondrial dysfunction only |
Key Procedure Step | Uses egg as-is | Replaces egg mitochondria pre-fertilization |
U.S. Legal Status | Widely available | Restricted, requires international travel |
Intended Outcome | Improved fertilization | Disease prevention & restored egg quality |
How IVF and MRT Work Differently
Standard IVF and mitochondrial replacement therapy follow similar initial pathways, but diverge significantly when it comes to genetic contributions and egg preparation. Understanding these mechanical differences helps explain why MRT offers solutions that standard IVF cannot.
In standard IVF, the process is straightforward. Your egg and your partner’s sperm meet in a laboratory dish outside your body. Fertilization occurs naturally between these two genetic sources. The resulting embryo develops for five to six days before transfer into your uterus.
Mitochondrial replacement therapy introduces a critical third genetic contributor. Instead of two genetic sources, your future child will inherit:
Nuclear DNA from your egg (containing most genetic information)
Nuclear DNA from your partner’s sperm
Mitochondrial DNA from a healthy donor egg
This three-parent genetics model is the defining characteristic of MRT. The donor’s mitochondria replace your faulty mitochondria, giving the embryo fresh cellular energy from the start.

The technical execution differs dramatically between these approaches. Specialized egg manipulation techniques like pronuclear transfer and maternal spindle transfer prepare your egg before fertilization even occurs. These steps add complexity that standard IVF never requires.
Here’s the timeline difference:
Standard IVF: Hormone stimulation → egg retrieval → fertilization → embryo development → transfer
Mitochondrial replacement therapy: Hormone stimulation → egg retrieval → mitochondrial DNA removal and replacement → fertilization → embryo development → transfer
That extra mitochondrial manipulation step occurs before sperm ever meets egg. Your egg is essentially “rebuilt” with new mitochondria before fertilization begins. This is why MRT requires specialized expertise and equipment.
The fundamental difference lies in timing: standard IVF works with your egg as-is, while MRT repairs your egg before fertilization to restore mitochondrial function.
For women over 40 with normal mitochondria, this extra step provides no benefit. Your standard IVF cycle proceeds efficiently without it. But for women whose eggs carry dysfunctional mitochondria, this preparatory step becomes essential.
Both approaches aim for the same outcome: a healthy embryo ready for implantation. The path to get there simply differs based on whether your fertility barrier involves mitochondrial dysfunction or other factors affecting egg quality and fertilization.
Pro tip: Discuss with your fertility specialist whether your specific infertility diagnosis warrants the additional complexity and cost of MRT preparation, or whether standard IVF modifications alone will address your egg quality concerns.
Health, Genetic, and Practical Benefits
Mitochondrial replacement therapy offers distinct advantages that standard IVF cannot provide, particularly for women with specific genetic and fertility challenges. These benefits extend beyond fertility to encompass your child’s long-term health and your family’s genetic legacy.
The most significant benefit is disease prevention. If you carry mitochondrial DNA mutations, standard IVF cannot protect your child from inheriting these mutations. Your biological eggs will always pass mutated mitochondria to the next generation. MRT changes this equation entirely by replacing your faulty mitochondria with healthy donor mitochondria before fertilization.
This genetic advantage prevents serious health complications:
Brain damage and cognitive impairment
Heart and cardiac dysfunction
Severe liver disease
Progressive muscle weakness and degeneration
Energy depletion affecting vital organs
These conditions are often life-limiting and severely impact quality of life. Preventing inherited mitochondrial diseases through MRT means your child avoids these devastating outcomes entirely.
Beyond disease prevention, MRT addresses a secondary benefit: improved egg quality. Women over 40 often experience both diminished egg quantity and compromised mitochondrial function. Fresh donor mitochondria can restore cellular energy production in your eggs, potentially improving fertilization rates and embryo development.
This fertility enhancement matters significantly for your success rates. Better mitochondrial function means better embryo quality, which translates to higher implantation success and lower miscarriage risk.
Practically, MRT preserves something precious: biological connection to your child. Egg donation provides genetic anonymity and removes biological connection entirely. Adoption is beautiful but involves no genetic link. MRT allows you to maintain your genetic legacy while protecting your child’s health.
MRT combines the genetic connection of biological parenthood with the health protection that standard IVF alone cannot offer.
Your child inherits your nuclear DNA, your partner’s nuclear DNA, and healthy mitochondria from a donor. The genetic relationship remains intact in the ways that matter most to you.
For women over 40 without mitochondrial mutations, these benefits don’t apply. Standard IVF remains your appropriate path forward. But for women with confirmed mitochondrial dysfunction, MRT addresses fertility barriers while eliminating inherited disease risks simultaneously.
Pro tip: Request genetic counseling and mitochondrial DNA testing before deciding between IVF and MRT; understanding your specific genetic status will clarify which treatment pathway offers the greatest health benefits for your unique situation.
Key Risks, Controversies, and Legal Status
Mitochondrial replacement therapy presents genuine scientific, ethical, and legal complexities that deserve careful consideration. Understanding these challenges helps you make an informed decision about whether MRT aligns with your values and circumstances.
The primary scientific concern centers on unknown long-term effects. Mitochondrial DNA from a donor introduces genetic material that has never been tested in your family’s biological history. We simply don’t know how this third-party mitochondria will interact with your nuclear DNA across decades of life. Children born from MRT are still relatively young, so long-term health data remains limited.
A secondary risk involves mitochondrial heteroplasmy, where both your original mutated mitochondria and the donor’s healthy mitochondria coexist in cells. This mixing could theoretically allow mutated mitochondria to resurface or cause unexpected cellular dysfunction. Clinical trials continue to monitor for this possibility, but the risk cannot be entirely eliminated.
Ethical debates focus on several contentious issues:
Germline modification creates permanent genetic changes passed to future generations
Three-genetic-parent embryos raise philosophical questions about identity and parenthood
Equity concerns arise when treatment costs limit access to wealthy populations
Debate over whether preventing mitochondrial disease justifies the unknown risks
The legal landscape varies dramatically worldwide. The United Kingdom and Australia have approved regulated MRT specifically for mitochondrial disease prevention. These countries maintain strict oversight and require demonstrated medical need before proceeding.
The United States effectively bans MRT research. Congressional restrictions prohibit FDA funding for MRT applications, making it unavailable domestically. This regulatory barrier exists despite no absolute safety ban—the restriction is primarily political and funding-based.
This legal disparity creates a critical reality for American women: accessing MRT requires traveling internationally, typically to countries like the Bahamas where the procedure is available and regulated. Cost considerations become substantial when international travel, accommodation, and specialized treatment are factored together.
The legal status of MRT determines not just availability, but affordability and accessibility for patients seeking this treatment option.
For women considering MRT, these complexities matter. You’re not choosing between proven options, but rather between established fertility treatments with known limitations and emerging treatments with unknown long-term outcomes.
Standard IVF carries its own risks—ovarian hyperstimulation, infection, bleeding—but decades of safety data exist. MRT offers potential benefits while introducing novel unknowns that clinical research is still evaluating.
Pro tip: Before pursuing MRT, request a detailed discussion with your fertility specialist about your specific risk factors, the regulatory status in your treatment location, and realistic long-term outcome expectations based on current clinical evidence rather than projected benefits.
Who Should Consider Each Approach
Choosing between standard IVF and mitochondrial replacement therapy depends on your specific fertility challenge, genetic risk factors, and personal circumstances. One approach isn’t universally better—the right choice matches your unique situation.
Standard IVF is appropriate for you if:
You have normal mitochondrial function but struggle with infertility from other causes. This includes blocked fallopian tubes, low sperm count, ovulation problems, or age-related diminished ovarian reserve without mitochondrial dysfunction. Standard IVF addresses these barriers effectively with established success rates and decades of safety data.
You’ve had previous IVF failures unrelated to mitochondrial issues. Repeat IVF cycles with protocol adjustments often improve outcomes for women whose previous cycles failed due to fertilization problems, poor embryo quality from non-mitochondrial causes, or uterine factors.
You carry no known mitochondrial DNA mutations. If genetic testing shows normal mitochondrial function, MRT offers no advantage and exposes you to unnecessary unknowns.
Mitochondrial replacement therapy is suited for you if:
You carry confirmed mitochondrial DNA mutations that cause severe inherited disease. MRT is specifically recommended for women at high risk of transmitting mitochondrial disease to offspring. This is the primary indication where MRT’s benefits clearly outweigh its risks.
You’ve experienced repeated IVF failures specifically linked to poor egg quality from mitochondrial dysfunction. Some women over 40 show both diminished ovarian reserve and compromised mitochondrial function affecting fertilization and embryo development. Fresh donor mitochondria may restore the cellular energy your eggs need.
You’re under age 45 with confirmed mitochondrial disease risk. Younger women face decades of reproductive years ahead; preventing disease transmission becomes increasingly valuable.
You’re willing to travel internationally for treatment. Since MRT is restricted in the United States, accessing it requires going to countries where it’s legally available and regulated, such as the Bahamas.
A comparison framework helps clarify your situation:
Genetic risk present? Standard IVF if no; MRT if yes
Mitochondrial dysfunction confirmed? Standard IVF if no; MRT consideration if yes
Previous IVF failures? Standard IVF with protocol modifications; MRT only if mitochondrial cause documented
Age and timeline? Standard IVF for most; MRT if mitochondrial risk and time-sensitive disease prevention needed
Your specific genetic and fertility diagnosis, not your age alone, determines whether standard IVF or MRT represents the appropriate treatment pathway.
Women over 40 without mitochondrial mutations benefit most from standard IVF with advanced embryo selection techniques. Women over 40 with confirmed mitochondrial dysfunction may gain significant advantage from MRT’s ability to restore egg quality while preventing disease transmission.
The decision ultimately rests on diagnostic clarity. Genetic counseling and mitochondrial DNA testing provide the foundation for choosing correctly.
Pro tip: Request comprehensive genetic testing and mitochondrial function assessment before committing to either treatment; knowing whether mitochondrial dysfunction is actually limiting your fertility prevents unnecessary intervention and ensures you pursue the approach most likely to succeed in your specific situation.
This summary highlights which patients are best suited for IVF or MRT based on age, diagnosis, and practical considerations:
Factor | Standard IVF | MRT |
Mitochondrial Function | Normal | Dysfunction documented |
Genetic Disease Risk | None | High mitochondrial mutation risk |
Previous IVF Failures | Non-mitochondrial causes | Mitochondrial cause confirmed |
Age Limit | Typically up to mid 40s | Under 45, with genetic risk |
Accessibility | U.S. clinics available | Requires international travel |
Discover Advanced Fertility Solutions Tailored to Your Needs
Understanding the critical differences between standard IVF and Mitochondrial Replacement Therapy (MRT) is the first step toward overcoming age-related infertility and mitochondrial dysfunction. If you are a woman over 40 facing diminished egg quality or mitochondrial DNA mutations, settling for traditional fertility treatments may not be enough. The challenge lies in restoring your egg’s cellular energy and preventing inherited mitochondrial diseases—complex issues that only specialized interventions like MRT can address.
At the Rejuvenating Fertility Center in the Bahamas, we specialize in cutting-edge therapies that go beyond conventional IVF. Led by Dr. Zaher Merhi, our expert team offers personalized care with advanced solutions such as Mitochondrial Replacement Therapy and stem cell treatments designed to rejuvenate your ovarian function and improve your chances of success.
Take control of your fertility journey now and explore options that truly match your unique diagnosis and goals. Visit Rejuvenating Fertility Center to schedule a consultation and learn how our revolutionary treatments can help you achieve a healthy pregnancy while preserving your genetic legacy. Don’t wait—your path to parenthood deserves the most advanced science available today.
Frequently Asked Questions
What is the primary difference between IVF and mitochondrial replacement therapy (MRT)?
The key difference lies in how they address infertility. IVF uses your own eggs and sperm to create embryos, while MRT replaces defective mitochondria in your eggs with healthy mitochondria from a donor before fertilization.
Who should consider mitochondrial replacement therapy (MRT)?
MRT is recommended for women with confirmed mitochondrial DNA mutations that could cause serious inherited diseases and for those who have experienced repeated IVF failures linked to mitochondrial dysfunction affecting egg quality.
What are the potential health benefits of mitochondrial replacement therapy compared to standard IVF?
MRT can prevent the transmission of inherited mitochondrial diseases and may improve egg quality by ensuring fresh, functional mitochondria are used, which can enhance fertilization rates and lower the risk of miscarriage.
What are the risks associated with mitochondrial replacement therapy (MRT)?
Risks include unknown long-term effects of introducing donor mitochondria, the potential for mitochondrial heteroplasmy where mutated and healthy mitochondria coexist, and ethical concerns regarding germline modification and access to treatment.
Recommended
Comments