Ovarian Rejuvenation Workflow for Improved Fertility Success
- Jan 20
- 7 min read

Facing a diagnosis of diminished ovarian reserve can feel overwhelming, especially when you have tried traditional fertility options without success. The chance to pursue innovative approaches like ovarian rejuvenation offers new hope in places such as leading international clinics. Before starting this advanced fertility journey, it is crucial to understand how eligibility is assessed and what personalized preparation involves so you can make empowered choices for your reproductive future.
Table of Contents
Quick Summary
Key Point | Explanation |
1. Comprehensive Eligibility Assessment Required | Begin by undergoing thorough diagnostic evaluations to determine candidacy for ovarian rejuvenation therapies. |
2. Personalized Therapy Selection is Critical | Choose the most suitable treatment based on individual health profile, age, and fertility goals for optimal results. |
3. Ongoing Monitoring Essential During Treatment | Regular assessments of hormonal levels and follicular development help tailor the therapy to your body’s responses. |
4. Multi-dimensional Evaluation of Treatment Success | Conduct thorough assessments post-therapy to evaluate changes in ovarian function and adjust future strategies accordingly. |
5. Continuous Follow-Up for Fertility Planning | Maintain a flexible fertility plan that adapts to personal needs and health status during follow-up consultations. |
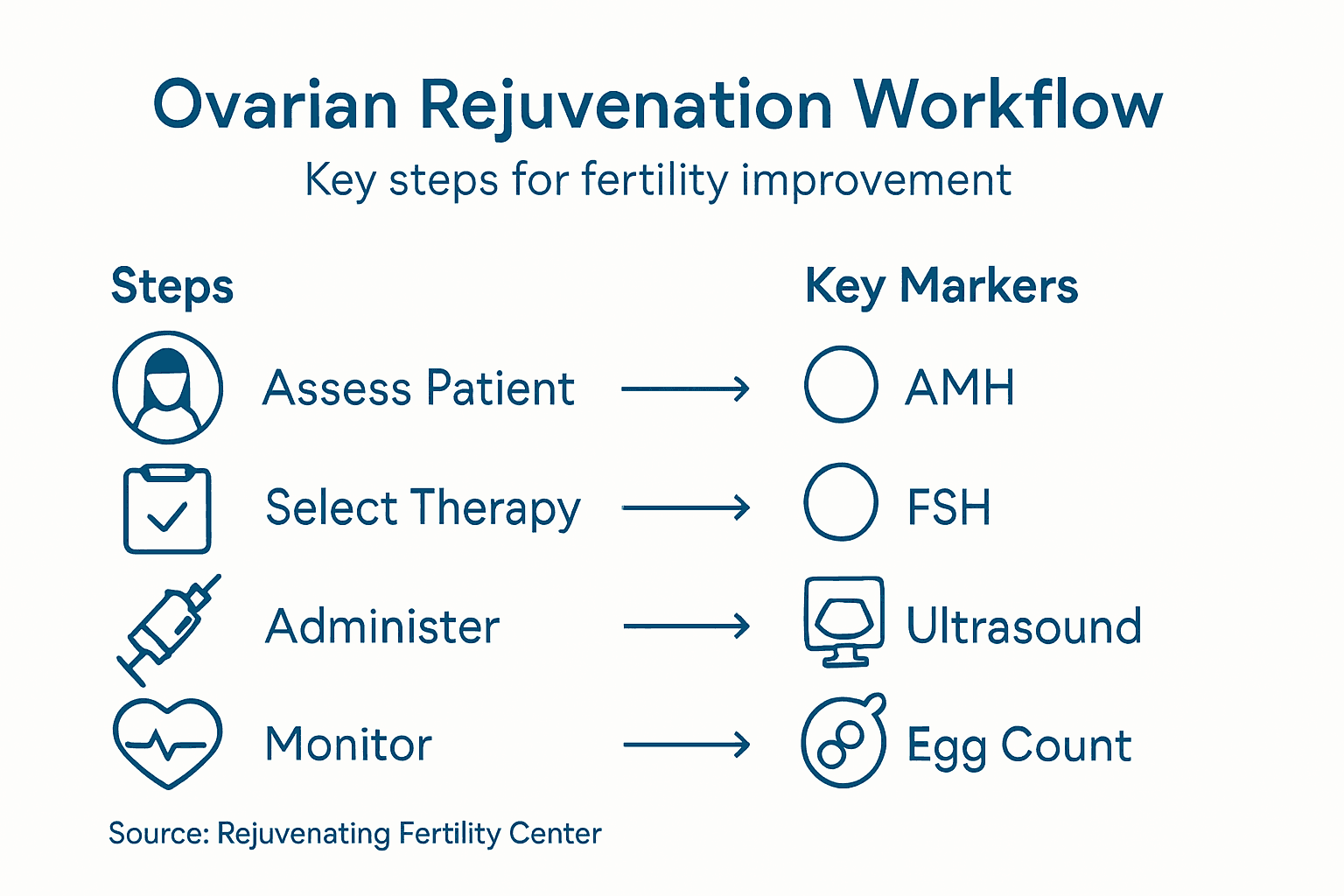
Step 1: Assess eligibility and prepare for ovarian rejuvenation
Navigating the complex world of ovarian rejuvenation begins with a thorough and personalized eligibility assessment. Your journey starts by understanding your unique reproductive health profile through comprehensive diagnostic evaluations that will determine your potential candidacy for this innovative fertility restoration approach.
Eligibility assessment involves multiple critical components. Physicians will conduct detailed hormonal marker analysis focusing on key indicators like anti-Müllerian hormone (AMH), follicle-stimulating hormone (FSH), and antral follicle count. These tests provide insights into your ovarian reserve and potential response to rejuvenation treatments. Your clinical history becomes crucial during this stage, with medical professionals examining factors such as age, previous fertility treatments, genetic predispositions, and overall reproductive health.
Preparation extends beyond medical testing and involves comprehensive patient counseling. Understanding realistic treatment outcomes, potential risks, and individual fertility potential forms the cornerstone of your preparation. Expect an in-depth discussion about your reproductive goals, lifestyle factors, and a personalized treatment strategy tailored specifically to your medical profile. This multidisciplinary approach ensures you have a holistic understanding of the ovarian rejuvenation process before proceeding.
Professional Advice: Schedule a comprehensive fertility consultation at least three months before considering ovarian rejuvenation to allow sufficient time for thorough diagnostic testing and personalized treatment planning.
Step 2: Select appropriate rejuvenation therapy tailored to needs
Selecting the most suitable ovarian rejuvenation therapy requires a nuanced understanding of your unique reproductive health profile and specific fertility goals. Your medical team will guide you through a comprehensive evaluation to determine the most effective personalized treatment approach that maximizes your chances of reproductive success.
The selection process involves carefully assessing multiple biological therapy options including platelet-rich plasma (PRP), stem cell therapy, in vitro activation (IVA), and mitochondrial targeting treatments. Each therapy offers distinct advantages depending on your specific ovarian function, residual follicle presence, and individual reproductive objectives. Physicians will conduct detailed diagnostic tests measuring key markers like anti-Müllerian hormone (AMH), follicle-stimulating hormone (FSH), and antral follicle count to recommend the most appropriate intervention.
Your personalized therapy selection will consider multiple critical factors beyond medical metrics. Age, previous fertility treatments, genetic predispositions, overall health status, and specific reproductive goals will all play significant roles in determining the most promising rejuvenation strategy. This comprehensive approach ensures that your chosen therapy aligns precisely with your individual needs and provides the highest potential for successful fertility restoration.
Here’s a quick comparison of leading ovarian rejuvenation therapies and their main attributes:
Therapy Type | Key Mechanism | Typical Candidates | Primary Consideration |
Platelet-Rich Plasma | Promotes tissue regeneration | Low ovarian reserve patients | Minimally invasive procedure |
Stem Cell Therapy | Cellular renewal stimulation | Severe ovarian insufficiency | Experimental, high potential |
In Vitro Activation | Activates dormant follicles | Younger women with follicles | May require surgical intervention |
Mitochondrial Therapy | Enhances cell energy output | Age-associated fertility decline | Supportive, adjunctive strategy |
Professional Advice: Request a comprehensive comparative analysis of potential rejuvenation therapies during your consultation to understand the specific benefits and potential outcomes for your unique reproductive profile.
Step 3: Administer therapy and monitor patient response
Once your personalized ovarian rejuvenation therapy is selected, the administration phase becomes a critical journey of precision and careful monitoring. Your medical team will implement the chosen treatment protocol with meticulous attention to detail, ensuring every aspect of the intervention is tailored to your unique physiological response.
The therapy administration involves precise biological treatment protocols designed to optimize your ovarian environment. Regular monitoring will include comprehensive diagnostic assessments tracking key indicators such as hormonal levels, ovarian reserve markers, and ultrasonographic follicular development. These detailed evaluations allow your healthcare providers to dynamically adjust treatment frequency, intensity, and approach based on your individual physiological responses and therapeutic progress.
Your medical team will establish a comprehensive monitoring schedule that extends beyond initial treatment administration. This will include periodic blood tests to assess hormonal changes, transvaginal ultrasounds to evaluate follicular development, and ongoing consultations to discuss your bodys response to the rejuvenation therapy. The goal is to create a responsive and adaptive treatment plan that maximizes your potential for improved reproductive outcomes while carefully managing any potential side effects or complications.
Professional Advice: Maintain a detailed personal health journal documenting any changes, symptoms, or physical sensations throughout your treatment to provide your medical team with comprehensive insights into your bodys response.
Step 4: Verify ovarian function and evaluate treatment results
Reaching the critical verification stage of your ovarian rejuvenation journey requires a comprehensive and nuanced approach to assessing your bodys response to treatment. This phase represents a pivotal moment where medical expertise transforms clinical data into meaningful insights about your reproductive potential.
Your medical team will conduct multi-dimensional functional assessments that go far beyond simple measurements. These evaluations will integrate biochemical markers, ultrasonographic imaging, hormonal profiles, and clinical observations to create a holistic picture of your ovarian recovery. Key diagnostic indicators will include anti-Müllerian hormone (AMH) levels, follicle-stimulating hormone (FSH), antral follicle count, ovarian volume, and critical fertility markers such as menstruation resumption and potential pregnancy outcomes.
The comprehensive evaluation process looks beyond isolated numbers to understand the comprehensive impact of your rejuvenation therapy. Your healthcare providers will analyze how treatment has potentially improved your ovarian reserve, follicular activity, and overall reproductive function. This thorough assessment helps determine the treatments effectiveness, provides insights into potential future fertility interventions, and allows for dynamic adjustments to your personalized reproductive care strategy.
Below is a summary of key diagnostic markers monitored throughout the ovarian rejuvenation process:
Diagnostic Marker | Purpose | Ideal Monitoring Stage |
Anti-Müllerian Hormone | Assess ovarian reserve | At baseline and follow-up |
Follicle-Stimulating Hormone | Evaluate ovarian function | Before and after therapy procedures |
Antral Follicle Count | Measure available follicles | Prior to therapy selection |
Ovarian Volume | Track ovarian health changes | During and post-intervention |
Professional Advice: Request a detailed written report of your functional assessment results to maintain a comprehensive understanding of your reproductive health progression.
Step 5: Schedule follow-up and adjust fertility strategy
The final stage of your ovarian rejuvenation journey involves strategic planning and continuous adaptation of your fertility approach. This critical phase transforms your initial treatment insights into a dynamic roadmap for future reproductive possibilities.
Your medical team will implement structured follow-up protocols designed to track your ongoing ovarian function and fertility potential. These scheduled appointments will involve comprehensive assessments including hormonal profile reviews, ovarian reserve biomarker analyses, and detailed discussions about your evolving reproductive goals. Depending on your initial treatment response, your healthcare providers may recommend adjustments such as transitioning to assisted reproductive technologies, modifying hormone replacement strategies, or exploring alternative fertility interventions.
The follow-up process is fundamentally personalized, recognizing that each womans reproductive journey is unique. Your medical team will collaborate closely with you to interpret diagnostic results, understand your emotional and physical responses to treatment, and develop a flexible fertility strategy that aligns with your personal timeline and reproductive aspirations. This approach ensures that your fertility plan remains responsive to your bodys changing needs and your individual life circumstances.
Professional Advice: Maintain a comprehensive medical record and fertility journal to facilitate more precise and personalized follow-up consultations with your healthcare team.
Take Control of Your Fertility Journey with Advanced Ovarian Rejuvenation at Rejuvenating Fertility Center
Struggling with low ovarian reserve or seeking innovative solutions to improve your reproductive potential can feel overwhelming. This detailed ovarian rejuvenation workflow highlights key challenges like assessing eligibility, selecting personalized therapies, and monitoring ovarian function to maximize fertility success. At Rejuvenating Fertility Center in The Bahamas, we specialize in cutting-edge treatments such as Mitochondrial Replacement Therapy and Stem Cell Therapy designed to restore ovarian function and enhance egg quality. Our expert team, led by Dr. Zaher Merhi, is dedicated to providing personalized care that aligns with your unique fertility goals.
Don’t let uncertainty hold you back from the family you dream of. Explore how our advanced ovarian rejuvenation therapies can offer new hope and measurable results. Visit Rejuvenating Fertility Center to learn more about our treatments and schedule a consultation. Discover personalized options including Mitochondrial Replacement Therapy and Stem Cell Therapy that can transform your fertility journey starting today.
Frequently Asked Questions
What is the eligibility assessment for ovarian rejuvenation?
To qualify for ovarian rejuvenation, you need a comprehensive eligibility assessment. Schedule a detailed hormonal marker analysis to check key indicators like anti-Müllerian hormone and follicle-stimulating hormone within the first few weeks of consultation.
How do I choose the right ovarian rejuvenation therapy?
Selecting the appropriate therapy involves evaluating your reproductive health profile and fertility goals. Consult with your medical team to discuss options such as platelet-rich plasma, stem cell therapy, or in vitro activation, ideally within a month of your eligibility assessment.
What monitoring is involved after administering ovarian rejuvenation therapy?
Following the therapy, your medical team will monitor your hormonal levels and follicular development through regular blood tests and ultrasounds. Ensure to keep a record of your symptoms and any changes, and expect to attend follow-up appointments every few weeks.
How are treatment results verified after ovarian rejuvenation?
Treatment results are verified through multi-dimensional assessments of ovarian function, including hormonal profiles and follicular activity. Request a comprehensive written report of your assessment results to understand your progress and potential next steps.
What should I do if my fertility strategy needs adjustment after my treatment?
If your initial treatment response indicates a need for changes, your medical team will propose modifications to your fertility strategy. Collaborate closely with your healthcare providers to review diagnostic results and adjust your plan, typically within two to three months after your evaluations.
Recommended
Comments