Personalized Fertility Treatment Doubles IVF Success for 40+
- Mar 2
- 10 min read

You’ve been told that fertility treatment success depends mainly on your age. What if the real difference lies in how your treatment is customized to your unique ovarian biology? Personalized fertility treatment transforms outcomes for women over 40 by tailoring protocols to individual ovarian reserve profiles, hormone levels, and egg quality markers. This guide reveals how personalization nearly doubles your chances of achieving pregnancy, even with diminished ovarian reserve.
Table of Contents
The Role of Diminished Ovarian Reserve in Fertility Personalization
Innovative Treatments: Mitochondrial Replacement and Stem Cell Therapy
Comparing Personalized vs Standard Fertility Treatment Protocols
Patient Assessment and Tailoring Personalized Fertility Protocols
Common Misconceptions About Personalized Fertility Treatment
Applying Personalized Fertility Treatment: What Women Over 40 Can Expect
Key Takeaways
Point | Details |
Personalized protocols adapt to your ovarian reserve | Treatments adjust based on AMH, FSH, and mitochondrial biomarkers rather than age alone. |
Advanced therapies enhance egg quality | Mitochondrial replacement and stem cell therapy target cellular energy and ovarian function. |
Success rates double with personalization | Personalized fertility treatment for diminished ovarian reserve increases live birth rates from under 10% to 20-30% for women over 40. |
Comprehensive diagnostics guide treatment | Hormonal, genetic, and mitochondrial assessments shape stimulation strategies and adjunct therapies. |
Ethical considerations remain central | Informed consent and thorough discussions ensure responsible use of innovative treatments. |
Understanding Personalized Fertility Treatment
Personalized fertility treatment tailors your care based on detailed biological ovarian profiles rather than generic age-based assumptions. Women over 40 often present with vastly different ovarian reserves, yet standard IVF protocols treat everyone identically, ignoring crucial biomarker variations that determine success.
Traditional one-size-fits-all IVF protocols apply fixed stimulation dosages and timing regardless of individual ovarian response. Personalized treatments tailor interventions based on detailed diagnostics beyond age-based assumptions, addressing your unique hormonal landscape and egg quality markers. This approach integrates comprehensive diagnostics, customized stimulation protocols, and targeted adjunct therapies to maximize your fertility potential.
Key components of personalization include:
Detailed diagnostic assessments measuring ovarian reserve, hormonal balance, and mitochondrial function
Customized stimulation protocols adjusting medication types, dosages, and timing based on real-time monitoring
Targeted adjunct therapies like mitochondrial support or ovarian rejuvenation techniques
Continuous cycle monitoring enabling protocol adjustments for optimal egg retrieval
Multidisciplinary care teams integrating reproductive endocrinology, genetics, and embryology expertise
Biological differences matter profoundly because your ovarian reserve and hormone levels dictate how you respond to stimulation. Exploring advanced fertility options reveals how advanced IVF options for women over 40 incorporate these individualized strategies, significantly improving outcomes. Understanding personalized fertility care impact helps you appreciate how tailored approaches transform success rates.
Pro Tip: Always ask your fertility specialist if your treatment is truly personalized or follows a generic protocol, requesting details on how your specific biomarkers shape your plan.
The Role of Diminished Ovarian Reserve in Fertility Personalization
Diminished ovarian reserve (DOR) describes reduced egg quantity and quality, a condition affecting most women over 40 to varying degrees. DOR dramatically lowers fertility success rates because fewer viable eggs are available for fertilization and embryo development.
Women over 40 with diminished ovarian reserve have IVF success rates under 10%, but personalized protocols increase live birth rates to approximately 20-30%. This near doubling of success stems from adjusting treatment protocols based on precise ovarian reserve measurements, including anti-Müllerian hormone (AMH) levels, follicle-stimulating hormone (FSH) concentrations, and antral follicle counts.
Personalization addresses DOR by customizing:
Hormonal stimulation dosages higher or lower depending on ovarian responsiveness
Medication timing synchronized with your natural hormonal cycles for optimal follicle recruitment
Adjunct therapies such as mitochondrial support supplements or growth hormone to improve egg quality
Cycle monitoring frequency increased to prevent over or under-stimulation and maximize egg retrieval
Embryo selection strategies prioritizing quality markers identified through preimplantation genetic testing
Comparing standard versus personalized treatment outcomes reveals striking differences:
Treatment Type | Live Birth Rate | Cycle Cancellation Rate | Average Eggs Retrieved |
Standard IVF Protocol | 8-10% | 35-40% | 3-5 eggs |
Personalized Protocol | 20-30% | 15-20% | 6-10 eggs |
Personalized care significantly reduces cycle cancellations by adapting stimulation strategies to your ovarian response. When you evaluate fertility treatments after 40, prioritizing personalized approaches ensures your diminished ovarian reserve is managed effectively rather than overlooked.
Innovative Treatments: Mitochondrial Replacement and Stem Cell Therapy
Mitochondrial replacement therapy (MRT) addresses cellular energy deficiencies that compromise egg quality as you age. Mitochondria generate the energy eggs need for successful fertilization and embryo development. MRT replaces defective mitochondria in your eggs with healthy donor mitochondria, boosting cellular energy and improving embryo viability.
Stem cell therapy for ovarian rejuvenation aims to restore ovarian function by introducing stem cells that may stimulate follicle development and hormone production. This experimental approach targets the root causes of ovarian aging, potentially increasing your egg production and improving overall reproductive capacity.
Benefits and outcomes of these therapies include:
Enhanced embryo quality leading to higher implantation rates
Increased number of viable eggs retrieved per cycle
Potential restoration of hormonal balance and menstrual regularity
Early clinical trials showing promising pregnancy rates, though long-term data remains limited
Availability in the Bahamas under specific regulatory frameworks permitting advanced reproductive technologies
The Bahamas provides a regulatory environment enabling access to these innovative therapies, offering international patients cutting-edge options not widely available elsewhere. However, ethical considerations in advanced fertility treatments remain paramount, requiring thorough informed consent discussions covering potential risks, success probabilities, and long-term implications.
Pro Tip: Discuss potential risks and ethical aspects thoroughly with your physician before opting for advanced therapies, ensuring you understand both the benefits and limitations based on current clinical evidence.
Exploring stem cell ovarian rejuvenation in Bahamas and learning how mitochondrial replacement therapy explained empowers you to make informed decisions about incorporating these innovations into your personalized treatment plan.
Comparing Personalized vs Standard Fertility Treatment Protocols
Understanding the differences between personalized and standard fertility treatment protocols clarifies how tailored approaches improve your outcomes. The comparison below highlights key distinctions:
Criteria | Standard Protocol | Personalized Protocol |
Treatment Assessment | Age-based protocols with minimal biomarker testing | Comprehensive diagnostics including AMH, FSH, mitochondrial DNA, and genetic screening |
Customization | Fixed stimulation dosages and timing | Dynamic adjustments based on real-time ovarian response monitoring |
Adjunct Therapies | Rarely incorporated | Mitochondrial support, stem cell therapy, growth hormone as indicated |
Success Rates (Live Birth) | 8-10% for women over 40 with DOR | 20-30% for women over 40 with DOR |
Cycle Cancellations | 35-40% due to poor response or over-stimulation | 15-20% with adaptive protocol modifications |
Ethical Considerations | Standard informed consent | Detailed discussions on novel therapies, risks, and long-term unknowns |
Personalized protocols use biomarker data to guide every treatment decision, while standard protocols default to age-based assumptions that ignore individual ovarian function. This biomarker-driven approach reduces cycle cancellations because your stimulation plan adapts to your ovarian response, preventing poor outcomes before they occur.
Personalized treatment protocols improve outcomes and reduce cancellations compared to standard IVF, though ethical considerations remain essential for novel therapies. Key ethical aspects include:
Informed consent ensuring you understand experimental therapy risks and benefits
Transparent communication about success probabilities based on current evidence
Multidisciplinary assessments involving reproductive endocrinologists, geneticists, and ethics committees
Continuous monitoring for adverse effects and long-term follow-up for mother and child health
The multidisciplinary approach ensures your treatment plan considers not just reproductive outcomes but also safety, ethics, and holistic well-being. Reviewing types of fertility treatments for women over 40 helps you appreciate how personalized protocols integrate diverse treatment modalities for optimal results.
Patient Assessment and Tailoring Personalized Fertility Protocols
Comprehensive diagnostics form the foundation of personalized fertility treatment, guiding every aspect of your protocol design. These assessments measure hormonal, genetic, and mitochondrial markers that reveal your ovarian function and predict treatment response.
Key diagnostic tests include:
AMH (anti-Müllerian hormone) quantifying your ovarian reserve and predicting egg yield
FSH (follicle-stimulating hormone) levels indicating ovarian responsiveness to stimulation
Mitochondrial DNA quantification assessing cellular energy capacity and egg quality potential
Genetic screening identifying chromosomal abnormalities or inherited conditions affecting fertility
Antral follicle counts via ultrasound visualizing available follicles for recruitment
Women over 40 receive hormonal, genetic, and mitochondrial assessments, including biomarkers like AMH, FSH, and mitochondrial DNA, to customize treatment. These biomarker results influence selection of ovarian stimulation methods, determining whether you receive mild stimulation to minimize side effects or aggressive protocols to maximize egg retrieval.
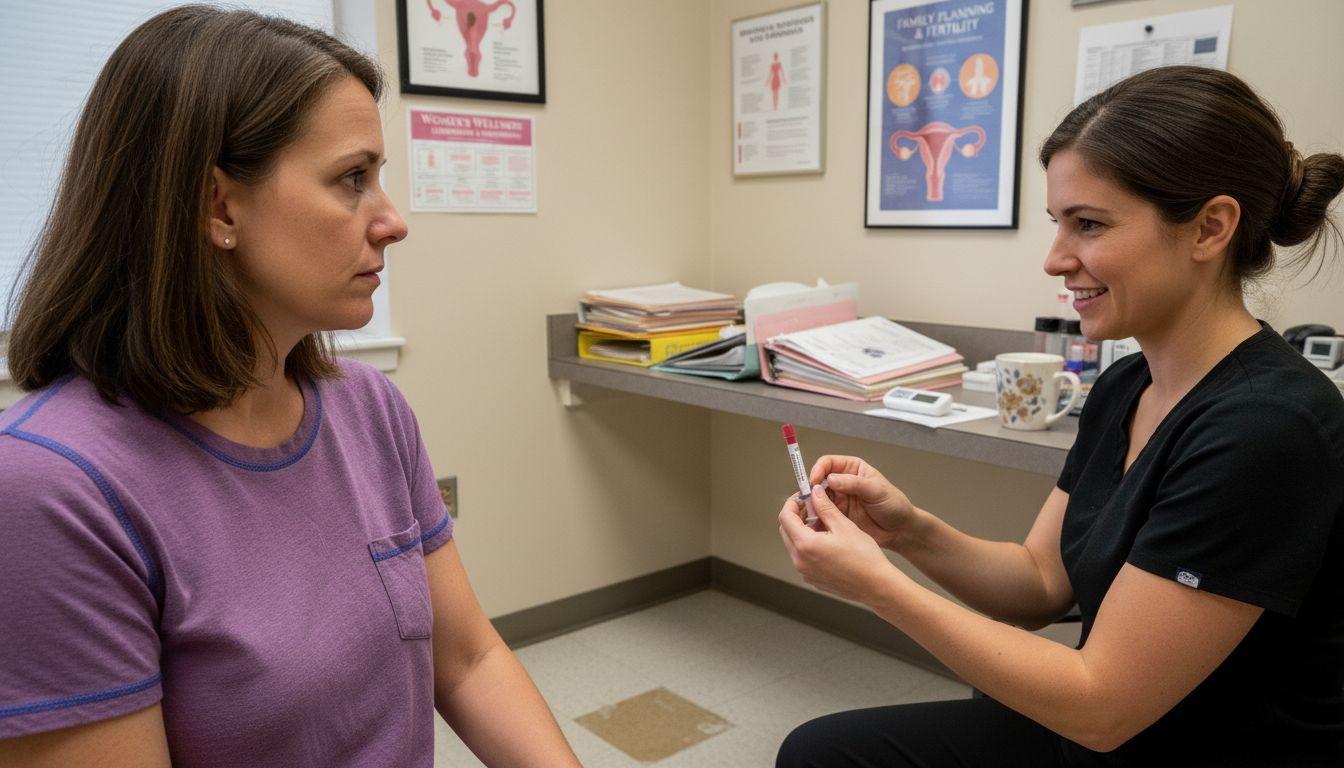
Continuous cycle monitoring tracks your response through serial ultrasounds and hormone measurements, enabling real-time dosage and timing adjustments. Your care team analyzes follicle growth patterns, estrogen levels, and ovulation timing to optimize egg maturity before retrieval.
The multidisciplinary team approach integrates reproductive endocrinologists, embryologists, genetic counselors, and nutritionists to address all facets of your fertility. This collaborative model ensures your treatment plan considers medical, genetic, and lifestyle factors, maximizing your chances of success. Exploring advanced IVF diagnostic options provides deeper insights into how these assessments shape your personalized protocol.
Common Misconceptions About Personalized Fertility Treatment
Misconceptions about fertility treatment can prevent you from pursuing effective personalized care. Clarifying these myths empowers you to make informed decisions based on evidence rather than assumptions.
Top myths versus facts:
Myth: All women over 40 have the same fertility chances. Fact: Not all women over 40 have equal fertility chances; personalized treatment adjusts for ovarian reserve variation, recognizing significant biological differences.
Myth: Personalized fertility treatment is just marketing jargon. Fact: Personalization is evidence-based tailoring using biomarker diagnostics, not superficial customization.
Myth: Diminished ovarian reserve means zero chance of pregnancy. Fact: Innovative treatments like mitochondrial replacement and stem cell therapy offer new hope, with success rates reaching 20-30%.
Myth: Advanced therapies are unsafe and unproven. Fact: Growing clinical support and ethical oversight guide responsible use, with early trials showing promising results.
Myth: Standard IVF protocols work fine for everyone. Fact: Standard protocols ignore individual ovarian function, leading to higher cancellation rates and lower success rates compared to personalized approaches.
Personalization involves rigorous scientific assessments that guide treatment decisions, not simply rebranding standard care. Diminished ovarian reserve reduces but does not eliminate your fertility potential, especially when innovative therapies target underlying cellular and hormonal deficiencies.
Rather than accepting oversimplified assumptions, seek detailed consultations to understand how personalized care addresses your unique fertility challenges. Understanding personalized fertility care impact helps you recognize the tangible benefits beyond marketing claims.
Applying Personalized Fertility Treatment: What Women Over 40 Can Expect
Entering personalized fertility care involves a structured process designed to maximize your chances of pregnancy while supporting your overall well-being. Here’s what you can expect:
Initial consultation: Comprehensive discussion of your medical history, fertility goals, and previous treatment experiences to establish baseline understanding.
Biomarker diagnostic testing: Blood tests measuring AMH, FSH, estradiol, and mitochondrial DNA, plus ultrasounds assessing antral follicle counts and ovarian structure.
Tailored protocol design: Your care team analyzes diagnostic results to create a customized stimulation plan specifying medication types, dosages, and timing.
Ovarian stimulation and monitoring: Daily or alternate-day injections combined with frequent ultrasounds and hormone measurements to track follicle development and adjust protocols.
Egg retrieval and fertilization: Surgical procedure to collect mature eggs, followed by fertilization using sperm from your partner or donor, with optional preimplantation genetic testing.
Embryo transfer and follow-up: Transfer of the highest quality embryo into your uterus, followed by pregnancy testing and ongoing monitoring if successful.
Success metrics you should expect include live birth rate improvements, reduced cycle cancellations, increased oocyte yield, and enhanced patient satisfaction. Personalized treatment includes comprehensive diagnostics and iterative treatment adjustments with measurable improvements in live birth rates and patient well-being.
Pro Tip: Maintain open communication with your care team to adjust treatments and manage expectations, ensuring you feel supported throughout the process.
Psychological support alongside medical treatment enhances your holistic well-being during the fertility journey. Counseling, support groups, and stress management techniques help you navigate the emotional challenges inherent in fertility treatment. Reviewing the step-by-step IVF process provides a detailed roadmap of what to anticipate at each stage.
Explore Personalized Fertility Solutions at RFC Bahamas
RFC Bahamas specializes in personalized fertility care and advanced therapies like mitochondrial replacement and stem cell therapy, offering you cutting-edge solutions tailored to women over 40 facing diminished ovarian reserve. Our multidisciplinary team integrates reproductive endocrinology, genetics, and embryology expertise to create individualized treatment plans that maximize your fertility potential.
Explore our comprehensive fertility treatment planning guide to understand how personalized protocols transform outcomes. Discover how mitochondrial replacement therapy in Bahamas enhances egg quality at the cellular level, and learn about stem cell ovarian rejuvenation services designed to restore ovarian function and boost your chances of pregnancy. Schedule a consultation today to access compassionate, evidence-based fertility care that adapts to your unique biology and goals.
Frequently Asked Questions
What does personalized fertility treatment involve for women over 40 with diminished ovarian reserve?
Personalized fertility treatment involves comprehensive diagnostics measuring your AMH, FSH, mitochondrial DNA, and antral follicle count to assess ovarian reserve and egg quality. Your care team designs a customized stimulation protocol adjusting medication types, dosages, and timing based on your biomarkers and real-time cycle monitoring, often incorporating adjunct therapies like mitochondrial support or stem cell therapy to enhance outcomes.
How can mitochondrial replacement therapy improve egg quality?
Mitochondrial replacement therapy replaces defective mitochondria in your eggs with healthy donor mitochondria, boosting cellular energy needed for successful fertilization and embryo development. This enhanced energy capacity improves embryo viability and implantation rates, addressing a key factor in age-related fertility decline.
What risks and ethical concerns are associated with advanced fertility therapies?
Advanced therapies like mitochondrial replacement and stem cell therapy carry risks including unknown long-term effects on offspring, variable success rates due to limited clinical data, and potential ovarian hyperstimulation or surgical complications. Ethical concerns involve informed consent, transparency about experimental status, and ensuring treatments are evidence-based rather than purely commercial, requiring thorough discussions with your care team and ethics committees.
How do success rates compare between personalized and standard treatments?
Personalized fertility treatments achieve live birth rates of 20-30% for women over 40 with diminished ovarian reserve, compared to 8-10% with standard IVF protocols. Personalized approaches also reduce cycle cancellation rates from 35-40% to 15-20% by adapting protocols to your ovarian response, significantly improving your chances of a successful pregnancy.
What should I expect during initial diagnostic assessments?
Initial diagnostic assessments include blood tests measuring hormones like AMH, FSH, and estradiol to evaluate ovarian reserve, plus transvaginal ultrasounds to count antral follicles and assess ovarian structure. You may also undergo mitochondrial DNA quantification and genetic screening to identify factors affecting egg quality and fertility potential, with results guiding your personalized treatment plan design.
Recommended

I tried an In Vitro Fertilization care service in London after finding it online, and the experience was smoother than expected. The guidance felt clear and reassuring.